Promoting Interoperability Overview
This documentation describes the workflows that Prime Suite users should implement in support of 2020 Promoting Interoperability (PI) measures for both Medicare and Medicaid reporting.
MIPS and Medicaid Measure Quick Start Guides
MIPS Promoting Interoperability Measures
Medicaid Promoting Interoperability Measures
This documentation describes the PI measures that are expected to be available for reporting in Prime Suite Reporting 2020.
Related Documentation
For information on the Promoting Interoperability programs, as well as the specifications for 2020 reporting, refer to the following pages on the Centers for Medicare & Medicaid Services (CMS) web site:
| Program | Resources |
|---|---|
| Medicare |
2020 Program Requirements Medicare Quality Payment Program - Promoting Interoperability Measures Requirements |
| Medicaid |
2020 Program Requirements Medicaid Your State Medicaid Agency: Check with the Medicaid Agency for your state for filing instructions, reporting deadlines, and any differences between the state and federal (CMS) Medicaid measure guidelines. |
Additional Notes
In this guide, the Definition of Terms sections contain terms and definitions from the CMS Promoting Interoperability specifications.
Qualification: The patient, prescription, order, summary of care document, or transition of care must qualify for the denominator of a measure to be considered for the numerator of that measure.
Visit requirement: The various PI measures may count entry types of patients, prescriptions, orders, or transitions of care, depending upon the measure. In general, for the entry to be considered for the denominator of a measure, the related patient must have had one non-voided face-to-face visit with an eligible provider (EP) or clinician. This visit must have been checked in during the measurement period. Additionally, the best practice is to ensure the visit is also checked out during the measurement period.
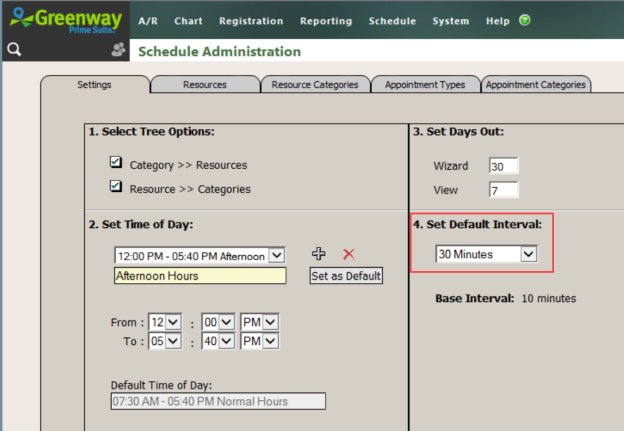
If a visit is not checked out, Prime Suite uses the Default Interval specified in Schedule Administration to determine the time to use as the end of the visit for calculations. The visit remains in a checked-in status.
Excluded Visit Types and Locations: In Prime Suite, you can exclude Visit Types and Locations from reporting in Prime Suite Reporting 2020 (PSR 2020). Visits can also be voided.
Visits saved with an excluded Visit Type, visits that occur at an excluded Location, and Voided visits are not included in the data sent to PSR 2020. Any actions that occurred during the visit cannot be used for qualifying patients. If something that would otherwise qualify for a measure occurs during a visit that is not sent to PSR 2020, the patient, prescription, order, summary of care document, or transition of care will not qualify.
Terminology Used in This Guide
See the following table for terminology used in this guide.
| Term | Description |
|---|---|
| API | A set of programming protocols established for multiple purposes. APIs may be enabled by a provider or provider organization to provide the patient with access to their health information through a third-party application with more flexibility than is often found in many current patient portals. |
| Business Days | Business Days are defined as Monday through Friday excluding federal or state holiday on which the EP or their respective administrative staffs are unavailable. |
| Measurement Period | From January 1st of the reporting year through December 31st of the reporting year. This cannot overlap calendar years. |
| Medicaid PI | Formerly called Meaningful Use (MU) Stage 3 |
| Performance Period | Typically used with MIPS; refers to the time frame used to report (any consecutive 90-day period or longer, up to a full calendar year). |
| PI | Promoting Interoperability |
| PI Transition, ACI Transition, or Meaningful Use Modified Stage 2 | These refer to older programs, which are no longer accepted by CMS and not available with Prime Suite Reporting 2020. |
| Reporting Period | Typically used with Medicaid; refers to the time frame used to report (any consecutive 90-day period or longer, up to a full calendar year). |
| Unique Patient | If a patient is seen by an EP more than once during the EHR reporting period, then for purposes of measurement, that patient is only counted once in the denominator for the measure. All the measures relying on the term unique patient relate to what is contained in the patient’s medical record. Not all of this information will need to be updated or even be needed by the provider at every patient visit. This is especially true for patients whose visit frequency is such that they would see the same provider multiple times in the same EHR reporting period. |

